Congratulations, you just hired a new employee, and they are excited about their dental benefits (hey, we are excited for them too). But before they take a seat in the dental chair, they may need to complete the new hire waiting period first.
How Long is a New Hire Waiting Period?
A new hire waiting period, is the required period of time that an employee will wait before their enrollment. The length of this waiting period can vary and is decided upon when your company applied for coverage with Dental Select. So, to avoid a lapse of coverage or unexpected expenses, it’s important to communicate this date to your new full-time employee.
Who is Eligible?
Full-Time employees
Generally, an employee is considered “full-time” if they work at least 30 hours per week and is on the regular payroll, but your company’s definition of full-time employment may differ. So, positions like independent contractors, temporary or seasonal workers, and part-time employees may not be eligible for coverage.
Dependents
Dependents who are eligible for coverage are decided upon in your certificate of insurance, but typically include the insured employee’s lawful spouse or dependent child (married or unmarried, up to the dependent age limit). Dependents may also include domestic partners, or any person related to the insured employee by blood or marriage.
When Can a New Hire Enroll?
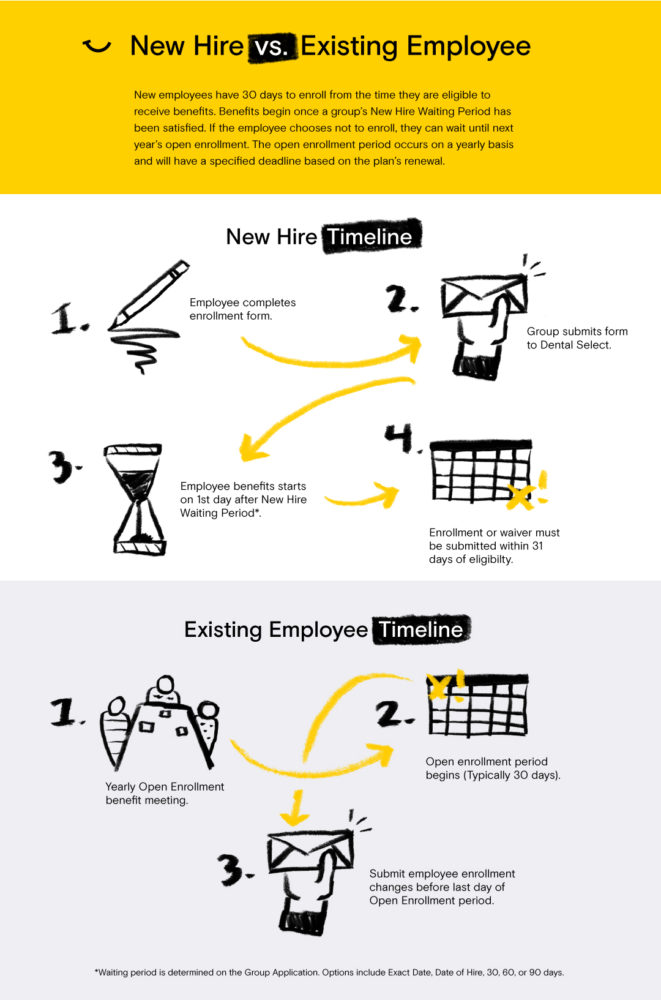
When your new hire employee enrolls on a Dental Select plan, benefits begin on the first of the month following a continuous full-time employment status and they’ve satisfied any required waiting period. Then, enrollment must be processed within 31 days of the day they become eligible.
To ensure timely enrollment, we strongly recommend you submit enrollment forms at the time of hire, rather than waiting until your employee has completed the new hire waiting period. That way, any possible delay in benefits can be avoided.
If your new employee chooses to waive their opportunity for benefits, they can wait to enroll in a future open enrollment or enroll within 30 days of a qualifying event. As a reminder, a qualifying event can be marriage, divorce or legal separation, birth of a child or adoption of a child, loss of employment, new employment, loss or gain of other coverage, or death of the insured.
For more information on the group enrollment process, here’s a little refresher.
