Log in to your new provider portal
If this is your first time logging in, use your Ameritas source code from an Ameritas EOP and follow the prompts to register. If you do not know your Ameritas source code, please contact customer service at 800-999-9789 or customercare@ameritas.com.
In the portal, you can access a range of features, including the updated provider guide, sample ID cards, fee schedules, patient benefit information, EOP statements, pre-treatment estimates, claim status, the new claims address, and payor ID.

How to navigate the portal resource center
1. Access patient benefit information
Select “Find a Member” at the top of page. Then, you can search for a member in three ways:
ID & Name
This is on the ID card or may be provided by the patient.
Claim number
Date of birth, name & state
This option works best if the member does not have their
ID card.


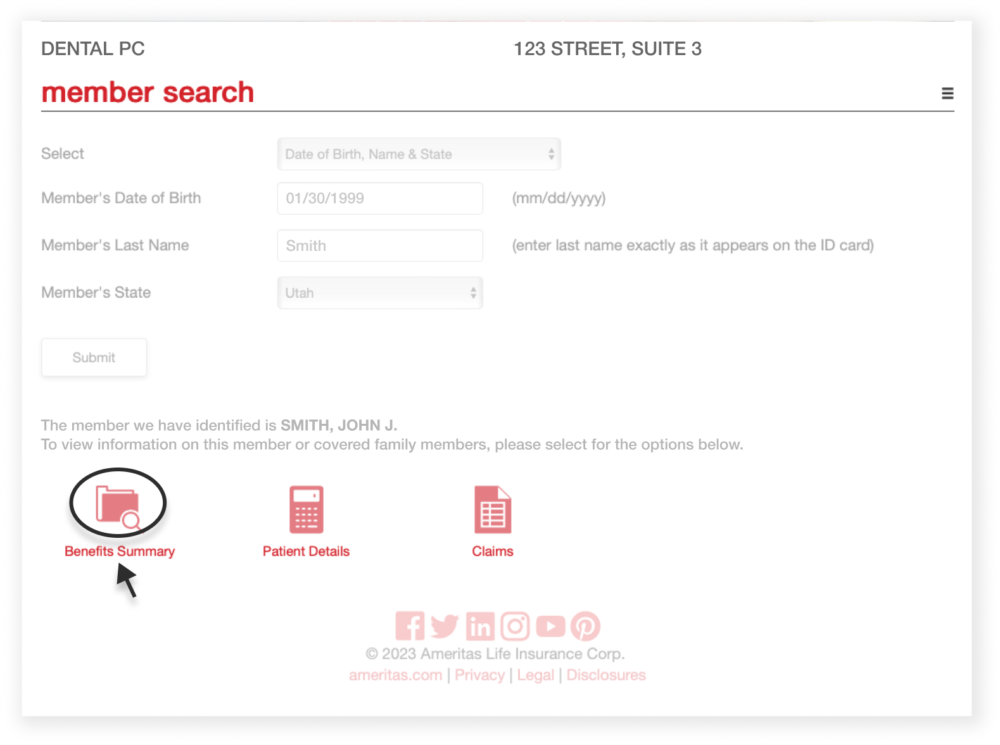
2. Locate the benefit summary
The comprehensive summary page will provide the plan number and procedure detail, including frequency.
Procedure details can be accessed after selecting “Benefits Summary” on the next page.
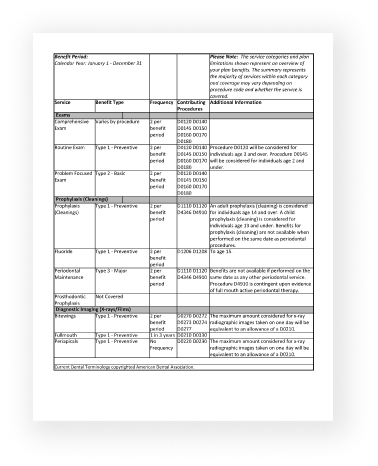
Sample Procedure Detail
Click to enlarge
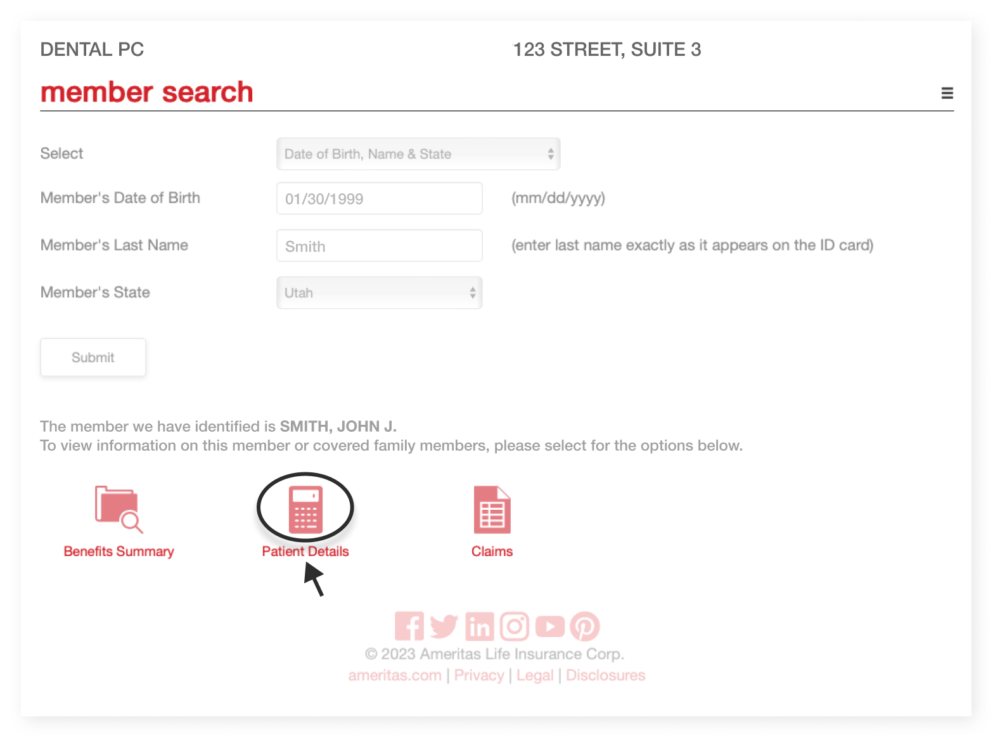
3. Retrieve patient details
Patient details will display an overview of the member, including member name, current status, plan sponsor, plan number, and coverage type.
Patient details can be accessed after selecting “Patient Details”.

Sample Patient Details
Click to enlarge
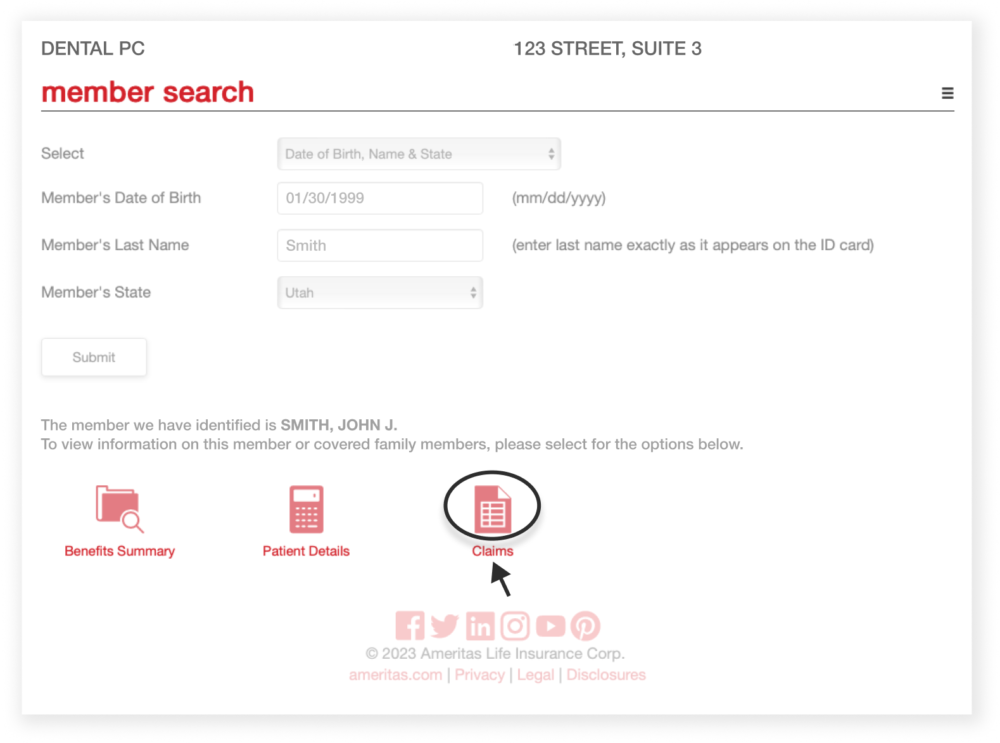
4. View claims
You can review pretreatment estimates and claim status for claims submitted on after June 30, 2023.
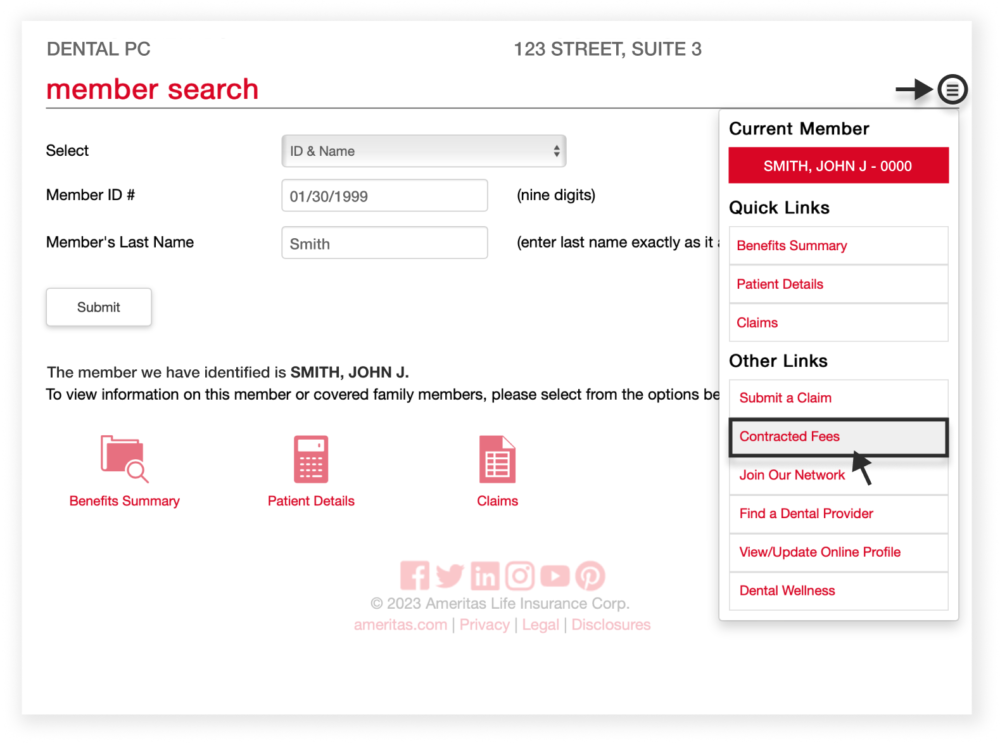
5. Download contracted fees
Access the fee schedules for your existing contracts, or download them into Excel in order to help you update your office records. Activate the dropdown menu and select “Contracted Fees” to download.
Dental Select fee schedules accessed from the provider portal will list the total provider fee. The Copay Plan fee schedules will be mailed annually.
Become a Provider
For nearly 35 years we’ve offered providers competitive network fees that rival other PPO plans, combined with our fast claim’s turnaround time. To join the Dental Select network, click below to send us your information, including address and phone number. Our provider relations team will then reach out to you to join the greatest dental network in America (yes, we’re a little biased).
Faster Claims Payments
Time is money. So don’t waste it waiting for claims payments. Take advantage of our electronic funds transfer solution.
Send Claims with EDI
Let our benefit experts help your practice become more efficient by using our standardized Electronic Data Interchange system to send claims electronically.
Automated FaxBack
Reduce the amount of time your office spends on administration by using our automated eligibility FaxBack system.
